Health
International law needed to combat superbug resistance: expert
Countries need to co-operate to ward off expected increase in deaths, says international lawyer and University of Ottawa professor

caption
International lawyer Steven Hoffman tries to lighten the mood with a “cuter superbug.”
caption
International lawyer Steven Hoffman tries to lighten the mood with a “cuter superbug.”Can international law be the weapon the world needs to win the war against superbugs? According to international lawyer Steven Hoffman, yes it can.
“Antimicrobial resistance will be one of the most defining health challenges (the world will) face over the next hundred years,” said Hoffman at a seminar hosted by the Dalhousie Health Law Institute on Friday.
“In order to solve the problem, all countries need to act. That seems like a good use for international law,” he said.
Over time, micro-organisms like bacteria, fungi, viruses and parasites can evolve to withstand antimicrobial drugs—medicines like antibiotics, antifungals, antivirals and antimalarials. This evolution occurs by chance, namely when micro-organisms try to replicate themselves and do so incorrectly.
Resistance is problematic because it reduces the effectiveness of standard medical treatments.
“Our use of antimicrobials significantly speeds the development of this resistance and is what allows (superbugs) to spread and proliferate globally,” said Hoffman. “When we take antibiotics in a hospital setting, we kill the bacteria still susceptible, leaving the bacteria that are resistant to stay. As a result, they then outcompete and multiply.”
Almost 700,000 people worldwide die of superbug infections each year—and this number is only going to increase. By 2050, experts predict nearly 10 million people will die each year of superbug complications. This will eclipse the number of deaths caused by cancer, heart disease or stroke.
According to Hoffman, the superbug problem has three parts:
- A lack of collective action among governing institutions
- The underprovision of antimicrobials in developing countries (and the overprovision of antimicrobials in developed countries)
- Insufficient innovation in the field: no new antibiotics have been developed in the last 20 years
Hoffman therefore advocates a three-pronged solution, one that encourages innovation in the field, promotes access to antimicrobials and conserves the effectiveness of existing drugs. Instituting an international legal framework, like a treaty, against antimicrobial resistance would force countries to commit to global, interdependent action.
“We need a mechanism whereby states can commit to each other,” he said. “That’s international law.”
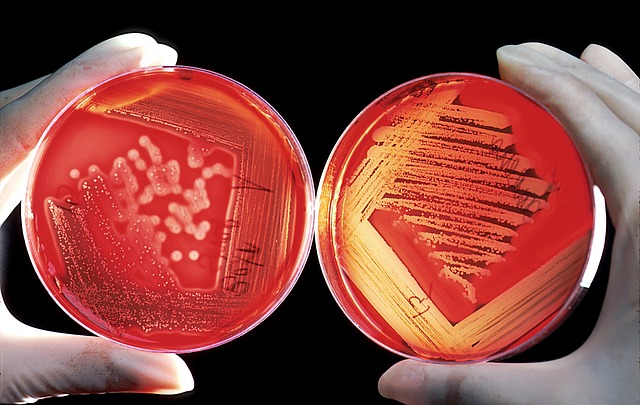
caption
Antimicrobial resistance is a global challenge, says Hoffman, one federal governments should be actively addressing.Some countries care more about access while other countries focus on innovation and conservation, he said. But countries need to address all three in order to solve the problem.
“Innovation without access is unjust, and innovation without conservation is wasteful,” said Hoffman.
Hoffman, director of the Global Strategy Lab at the University of Ottawa, says most people don’t recognize the problem of antimicrobial resistance, or AMR, because there’s no face behind the campaign.
“There’s a bit of a PR problem in this challenge,” said Hoffman. “When someone dies from an infection, we call it an infection. We blame that. We don’t usually say it was resistance to the drugs.”
But the dangers of antimicrobial resistance are everywhere. On Feb. 18, 2015, the Ronald Reagan UCLA Medical Center announced that nearly 100 liver, bile duct and pancreas patients may have been infected with a superbug during a diagnostic endoscopic procedure. Two of these patients later died. The resistant bacteria involved was transmitted through an inadequately disinfected scope.
Almost a year later, on Jan. 8, 2016, The Center for Infectious Disease Research and Policy in Minnesota reported the “newly identified” MCR-1 gene had been discovered in six new countries: Germany, Vietnam, Cambodia, Japan, Switzerland and Belgium, raising the total number of countries affected to 17. The gene makes E.coli resistant to a last-resort antibiotic.
But some medical professionals are skeptical of a legal approach. Janice Graham, a professor of Medical Anthropology and Infectious Diseases at Dalhousie University, says “it’s fine and well to talk about the governance of this, but even in Canada we know…the chance of getting (a preventative policy) through, until there’s a major international pandemic-type of event, is not going to happen.”
In the interim, Hoffman suggests:
- Regulating antimicrobial availability and prescription access
- Increasing the surveillance of antimicrobial use
- Prohibiting the marketing of antimicrobials
- Spending public money to incentivize innovation
“It’s clear we cannot just tackle the biological and clinical manifestation of this challenge,” said Hoffman. “We also need to tackle this difficult global, political challenge with action. We’re starting to think that an international treaty could provide legal protection against this challenge that is currently risking our collective well being, now and in the future.”

