Halifax college student hospitalized after drink spiked downtown
‘My feet felt like they were bolted to the floor,’ said Josée Saulnier

caption
Photo illustration of drink tamperingJosée Saulnier’s birthday celebration ended early when she found herself in need of a doctor.
Saulnier, a student at Nova Scotia Community College, was celebrating her 20th birthday with friends on Jan. 17. After spending some time at The Dome Nightclub in downtown Halifax, she started feeling unwell and decided to leave.
“I knew something was wrong,” she said.
Her friends called an ambulance because she was having full-body tremors. She also scratched her limbs uncontrollably despite not being itchy. Related stories
She said she had “no control” of her body, even though she only had three mixed drinks and a shot that night.
“I’m very careful when I’m drinking,” she said. “I have absolutely no idea how it could’ve happened.”
Saulnier was given an EKG at the QEII Health Sciences Centre’s emergency department. The doctor said it was either alcohol poisoning or drink tampering. There was nothing they could do, so they sent her home.
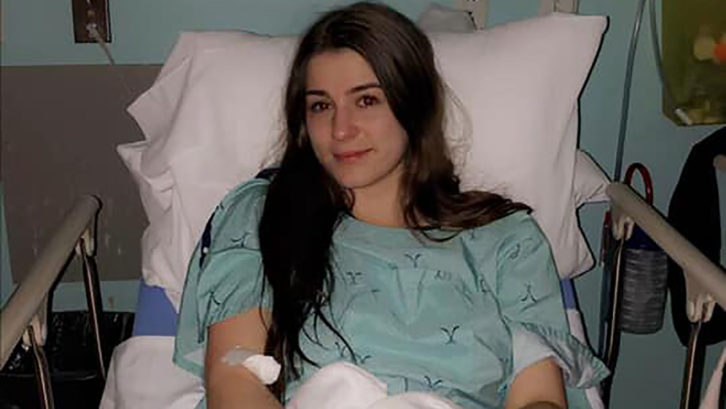
caption
The next morning, her symptoms came into full effect. Her tremors were stronger and she had blurry vision and slurred speech.
“I knew my body was in need of professional help,” she said.
An ambulance was called for the second time.
“As soon as I had seen the paramedics and police, I said, ‘This is what I need. I needed to be in their care,’” Saulnier said.
When she got to the hospital, she was told she was experiencing the effects of drink tampering. She was given Valium as a muscle relaxer, but it didn’t work so they had to increase her dosage.
Saulnier was then told to wait until the drug flushed out of her system.
Later that day, her symptoms worsened to the point that she was unable to walk. She said when her friends would try to help her stand, her feet wouldn’t move.
“My feet felt like they were bolted to the floor,” she said.
The Signal contacted The Dome for a comment and left a voicemail, but did not receive response by the end of the day.
Drink tampering not tracked
It’s unclear how often drink tampering occurs in Halifax. In an email, Dr. Kirk Magee, the zone chief for the QEII’s emergency department, said drink tampering incidents are not recorded.
“We do not formally track specific disease presentations to the emergency department unless it is part of the Clinician Quality and Innovation (CQI) process or an ongoing research project,” Magee said.
Patients with suspected drink tampering are treated the same as any patient with a suspected toxic ingestion.
“We would appropriately resuscitate the patient and investigate. There would be no specific additional investigations for this group of patients,” Magee said.
He said it’s not about what brought the patient into the emergency department, it’s about making the patient feeling better.
Since the incident, Saulnier said she is feeling a lot better and has reported the incident to the Halifax Regional Police.
Halifax Regional Police Const. John MacLeod said in an email: “We encourage anyone who believes they have been a victim of drink tampering to seek medical attention for their safety and contact police so that we are aware of it and can investigate the incident thoroughly.”
MacLeod said the RCMP conducted research for Halifax Regional Municipality (HRM) in June 2018 to identify drink tampering incidents and whether or not they should keep records. He said the RCMP found that “there wasn’t a sufficient basis for drink tampering to be tracked as a separate data category or crime trend.”
Incidents of drink tampering can’t be reported online. MacLeod said people must contact the non-emergency line to make the report or call 911 if the incident is in progress.

caption
The Dome Nightclub in downtown HalifaxDrink tampering ‘prevalent’
Saulnier posted her story on Facebook to warn others about the incident.
“I’m glad it happened to me because somebody else might’ve not had friends with them,” she said. “If I didn’t have friends with me, I guarantee that something worse would’ve happened.”
The 2018 to 2019 Sexual Assault Nurse Examiner (SANE) report for Halifax-based Avalon Sexual Assault Centre said one of the most significant risk factors for sexual assault was the use of alcohol.
The report found alcohol to be the most common substance used in drug-facilitated sexual assault. Drug-facilitated assaults can cause clients to have partial or complete memory loss, which could reduce the chances of the assault being reported.
Their research found that approximately 13 per cent of SANE clients “had no recall of the offender, often consistent with drugging or alcohol intoxication.”
The statistics are specific to the SANE program, which helps clients who call up to five days after the assault occurs.
Jackie Stevens, Avalon’s executive director, said there are multiple ways people are targeted and some are deliberately attempting to commit sexual offences by using alcohol and drugs.
Stevens reminds people that it is a criminal offence to unknowingly drug someone.
The section in Canada’s Criminal Code pertaining to administering noxious things states that states “every person who administers or causes to be administered to any other person or causes any other person to take poison or any other destructive or noxious thing is guilty.”
Stevens thinks tracking instances of drink tampering could prove useful.
“It’s worth considering tracking the numbers because there is a prevalence of people deliberately targeting people with drugs and alcohol tampering,” she said.
“It might help to track them in terms of understanding how prevalent it is and how we can address it.”
About the author
Lesli Tathum
Lesli is from the Cayman Islands. She is in her fourth year of journalism at the University of King's College and is a member of the King's Women's...
